During this wonderful time of year, protect your skin
Summer is almost over *sigh*. For many of us, the end of summer means we must bid a temporary farewell to Rhode Island’s beautiful beaches until next year. As wonderful as carefree summer days …
This item is available in full to subscribers.
Please log in to continue |
Register to post eventsIf you'd like to post an event to our calendar, you can create a free account by clicking here. Note that free accounts do not have access to our subscriber-only content. |
Day pass subscribers
Are you a day pass subscriber who needs to log in? Click here to continue.
During this wonderful time of year, protect your skin
Summer is almost over *sigh*. For many of us, the end of summer means we must bid a temporary farewell to Rhode Island’s beautiful beaches until next year. As wonderful as carefree summer days in sun may be, if we’re not careful, one might pay for it down the road with damaged skin cells. Damaged skin cells repeatedly exposed to the sun over many years (think about when you were in your teens and twenties) may become unruly and cancerous growths.
The most common skin cancer is Basal Cell Carcinoma (BCC). These are often found in sun exposed body parts, including the eyelids if you don’t wear sunglasses. There are four main subtypes of BCCs: super cial, nodular, in ltrative, and pigmented. Nodular subtypes are the most common type of BCC, but pigmented BCCs are the most common in patients of African, Asian and Hispanic descent. Because nodular BCCs are the most common, I will talk about those.
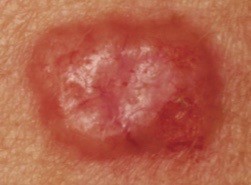
As mentioned above, basal cell carcinomas are most commonly found on sun exposed skin. Those who have spent extended time in the sun, are older, and/or have fair skin are more likely to develop this type of skin cancer. Patients who have had radiation treatments, a decreased immune system or a history of previous non-melanoma skin cancer are also at an increased risk. Nodular BCCs generally show up as pimple-like growths that don’t go away. They are pink, shiny, tend to have little blood vessels (telangiectasia) and can develop crusts or bleed easily. If you are unsure if the lesion you have is a BCC, it is best to have it evaluated by a dermatology health care provider. Some lesions are diagnosed by sight alone, however, if there is any uncertainty, a skin biopsy will likely be performed to confirm diagnosis.
Once a BCC diagnosis is made, a treatment plan will be established. Depending on site (where on your body the lesion is), cosmetic concern, BCC subtype, and the patient’s wound healing ability, the treatment plan will vary. Some options include: chemotherapy cream, liquid nitrogen, electrodessication and cur- retage (scraping and buring procedure), excision, radiation, Mohs surgery (surgical option where the tissue is examined during the procedure which allows for the least possible amount of skin to be removed), and pathway inhibitor pills (Erivedge, Odomzo). Your dermatology health care provider will discuss treatment options with you and together you will develop the most appropriate treatment plan.
Early detection and complete removal of a BCC provide a very high rate of success. Once you have been diagnosed with a BCC, you are at an increased risk of developing more. Twice yearly skin exams are highly recommended, along with regular self skin monitoring at home. Please contact your dermatology health care provider if you have new or changing lesions, and have them evaluated.
Remember, the best way to combat BCCs is to wear spf clothing and diligently apply sunscreen every two hours when you are exposed to the sun. If you are swimming, reapply every time you get out of the water. Sunscreen reapplication is so important, even on cloudy and winter days ... but now is not the time to talk about the “W” word.
Meighan Dingle Blanco, FNP-BC is a nurse practitioner with South County Dermatology.